On this page we discuss the care and support you can expect if you may be reaching the end of your life. If you have any questions about any of the topics we cover in this section, you can contact us or you may prefer to discuss them with your care team.
Life Expectancy and End of Life Considerations
Understanding life expectancy can be a significant concern for those living with neuroendocrine cancer. While not everyone with this disease will succumb to it, there comes a point when further treatment may not be effective. If you’re wondering about your life expectancy, it’s essential to discuss this with your healthcare team. They can provide personalised insights based on your specific circumstances, including the stage of your cancer, its aggressiveness, and your overall health.
Receiving news about reaching this stage can evoke a range of emotions, from shock to relief to disbelief. It’s entirely normal to feel overwhelmed or numb when facing such information. Remember, there’s no right or wrong way to respond, and it’s okay to seek support from loved ones or professionals during this time.
Additionally, end-of-life care should focus on ensuring you live as well as possible until the end, with dignity and in accordance with your wishes. If you have questions or concerns about end-of-life care, don’t hesitate to reach out to us or your healthcare team for guidance and assistance.
End-of-Life Support for Neuroendocrine Cancer Patients and Their Families
Dealing with end-of-life concerns and the loss of a loved one can be immensely challenging. At Neuroendocrine Cancer UK, we’re here to provide support and guidance every step of the way. Whether you’re facing a terminal diagnosis, concerned about what to expect in the final stages, or coping with the loss of someone dear, we’re here to offer comfort and assistance.
Support for Patients

Understanding Life Expectancy with Neuroendocrine Cancer
Neuroendocrine cancer is a complex condition, and life expectancy can vary greatly depending on various factors, including the type and stage of the cancer, treatment options, and individual health circumstances. It’s essential to have open and honest discussions with your healthcare team to understand what to expect and to make informed decisions about your care.
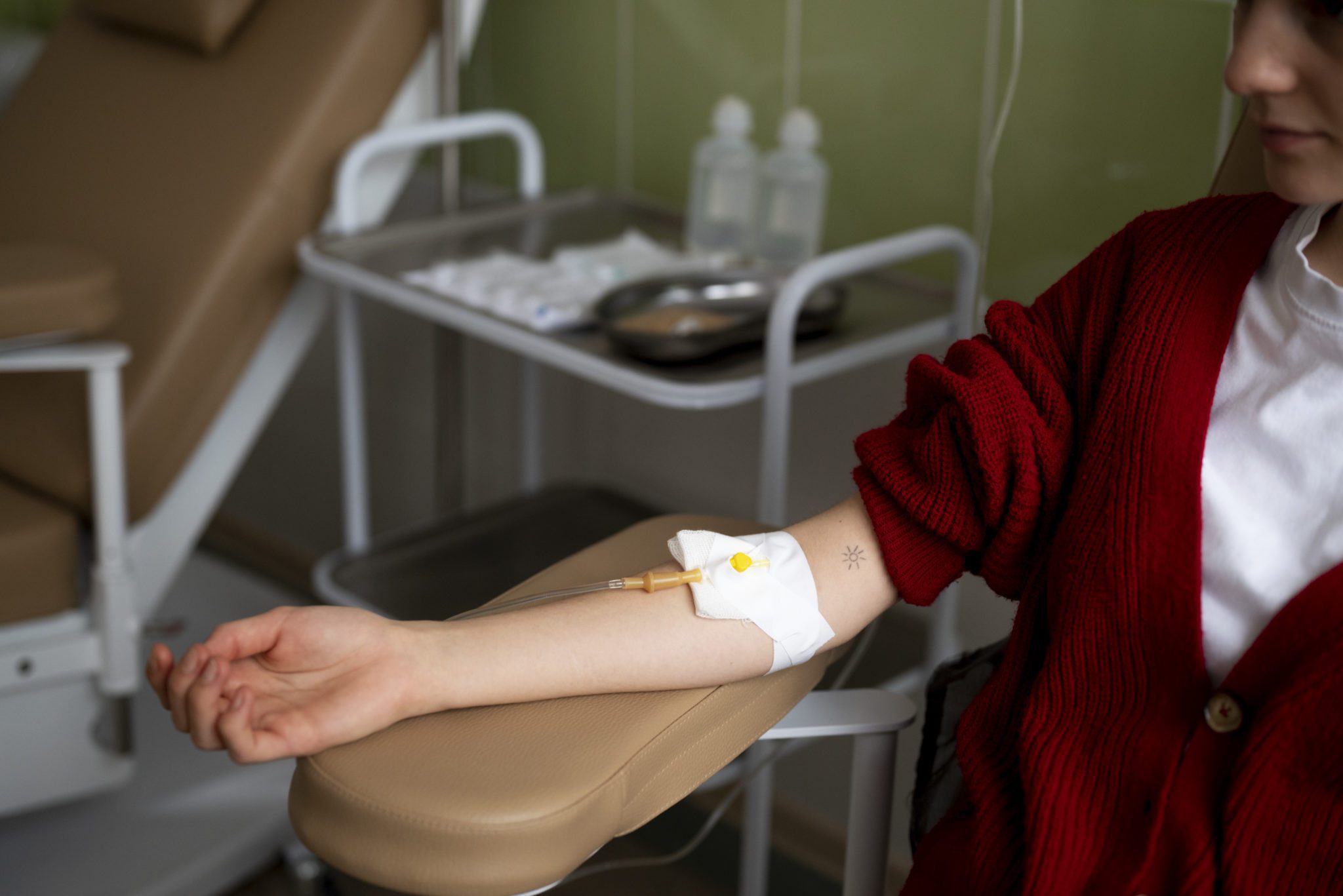
Advanced Disease – When Treatment is No Longer Working
As neuroendocrine cancer progresses and standard treatments become less effective, individuals may face the reality that their disease is advancing despite medical intervention. This phase, often termed advanced disease, presents unique challenges as symptoms may intensify and treatment options diminish. At this stage, the focus of care shifts towards symptom management and optimising quality of life. While confronting the limitations of treatment can be difficult, it’s essential for patients and their loved ones to engage in open and honest discussions with their healthcare team to explore available options, address concerns, and ensure their preferences guide the course of care.

Advanced Illness – Healthcare Support
In advanced illness, such as neuroendocrine cancer, decision-making is vital for aligning care with patients’ preferences. Healthcare professionals guide and support patients, ensuring their voices are heard and treatment preferences respected. By fostering open communication and providing emotional support, professionals empower patients to make informed choices, enhancing their autonomy and well-being throughout their journey.

Advance Care Plans (ACPs)
End-of-life care aims to ensure a dignified and comfortable transition, respecting your preferences and wishes. Your care team collaborates with you to plan personaliSed care that addresses physical, psychological, social, and spiritual needs. Whether at home, in a care facility, hospital, or hospice, the focus remains on enhancing your quality of life until the end. Advance Care Plans (ACPs) allow you to document treatment preferences, ensuring your wishes are honoured. For more details on advanced care planning and end-of-life care
Aura simplifies end-of-life planning by providing an online platform for you and your loved ones to organise crucial information, express wishes, document life stories, and schedule future messages.

End-of-Life Care and Support
For those approaching the end of life, palliative care plays a crucial role in providing comfort, managing symptoms, and supporting both patients and their families. Our team can provide information about available resources, including hospice care, pain management techniques, and emotional support services.
ReSPECT?
ReSPECT stands for Recommended Summary Plan for Emergency Care and Treatment. The ReSPECT process creates a personalised recommendation for your clinical care in emergency situations where you are not able to make decisions or express your wishes.

What Happens When I Die?
Facing mortality can be overwhelming, especially for someone living with neuroendocrine cancer. It’s natural to feel scared and anxious about what will happen when you’re no longer here. It’s important to know that you’re not alone. We, along with your healthcare team are here to provide support and guidance to help you navigate these difficult discussions and decisions. Additionally, reaching out to loved ones and seeking emotional support from our counsellors or support groups can provide comfort and reassurance during this challenging time. Remember that it’s okay to feel scared, but you don’t have to face these uncertainties alone.
Support for Family and Friends

An End-of-Life Diagnosis
When a loved one receives an end-of-life diagnosis, it can be an emotionally overwhelming and daunting time. Our support services are here to offer compassionate guidance and a listening ear to both you and your loved one as you navigate this challenging journey together. We understand the importance of providing support tailored to your specific needs during this sensitive time. Whether you need assistance understanding medical information, coping strategies, or simply someone to talk to, our helpline and counselling services are available to provide the support and reassurance you need.

Coping with Loss and Grief
Navigating the loss of a loved one to neuroendocrine cancer can be a profound and challenging experience. In recognition of this, our support services encompass grief and loss, providing compassionate assistance and a supportive presence to those who are grieving. Whether you need a listening ear or guidance through the grieving process, our helpline and counselling services are available to offer support to help you cope with your loss.

Neuroendocrine Cancer UK Remembers
Our Neuroendocrine Cancer UK Remembers page provides a special space for those who have lost a loved one to neuroendocrine cancer to honor and remember them. Here, you can create a memorial page dedicated to your loved one, where you can share memories, photos, and messages to commemorate their life and legacy. It’s a place where you can connect with others who understand your journey and find comfort in knowing that you’re not alone in your grief. Creating a memorial page allows you to celebrate the life of your loved one in a meaningful way and keep their memory alive for years to come.
