Metastatic disease
SECONDARY NEUROENDOCRINE CANCER
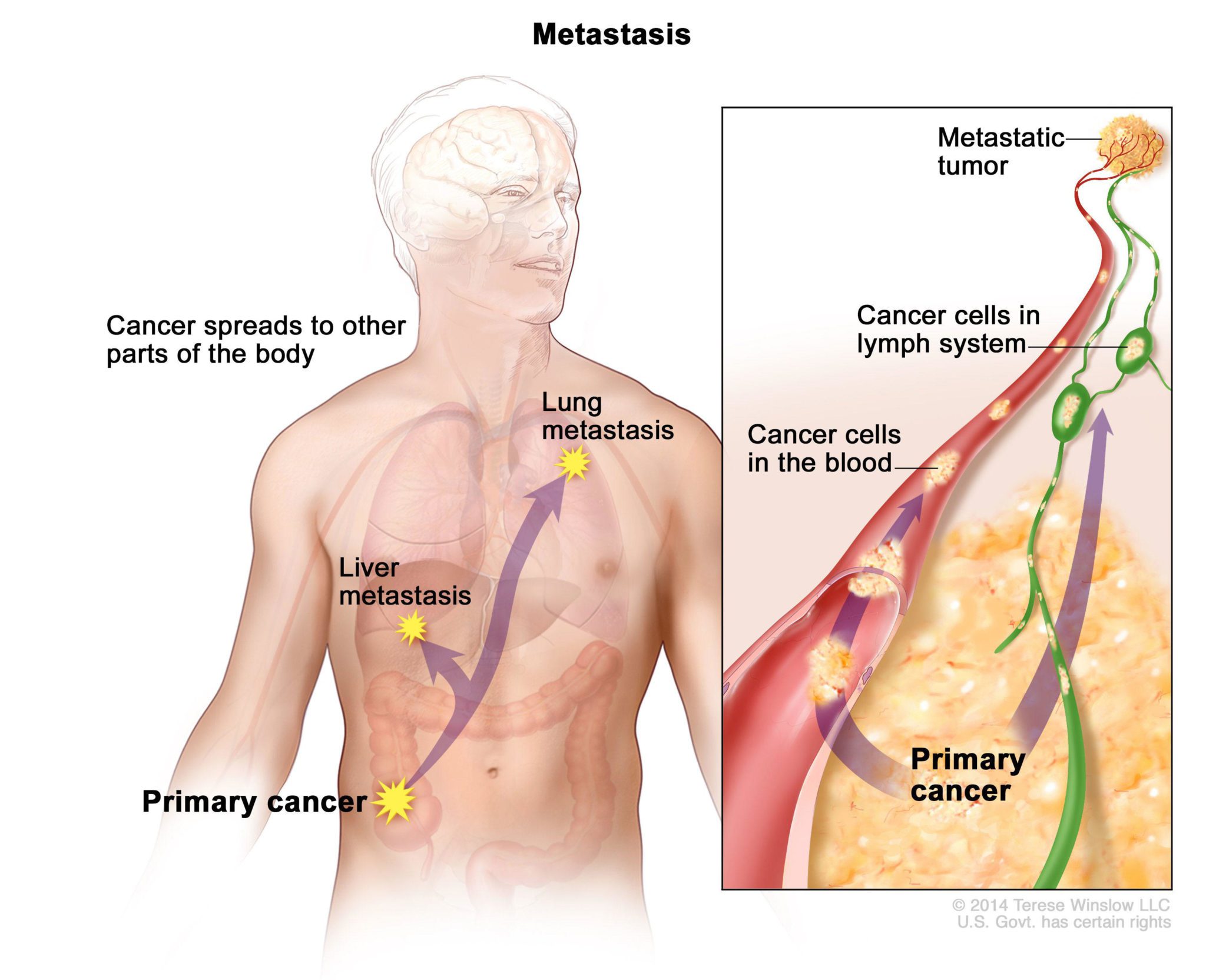
The terms ‘metastatic’ or ‘secondary cancer’ both refer to the spread of cancer cells from the place where they first formed (primary site) to another part of the body.
In metastastic or secondary disease, the cancer cells break away from the original (primary) cancer, travel through the blood or lymph system, and form a new site of disease in other organs or tissues of the body. This new site is called a metastatic or secondary site – and will be formed by the same kind of cancer cells as those found in the primary site. For example – if your primary site is the small bowel and you have metastases in the liver – the metastases will be formed by cancer cells from the small bowel, rather than liver cells.
f these cells form a single secondary tumour, that tumour is called a metastasis, if they form more than one tumour at one or more secondary sites, these secondary tumours are called metastases.
The liver is one of the most common sites for many Neuroendocrine Cancers to metastasise (spread) to, with primary liver Neuroendocrine Cancer being incredibly rare.
Most primary liver cancers start within the cells of the liver and / or bile ducts and are a completely different type of cancer – further information on Primary Liver Cancers that are not Neuroendocrine or Neuroendocrine Cancer-related can be found here.
Please note:
The spread of Neuroendocrine Cancer is not always a sign of rapid or aggressive cancer – nor is it necessarily a sign of end-stage/terminal disease. Metastatic cancer cells can also remain inactive at a distant site for many years before they begin to grow again, if at all.
Where a small, slow growing , low grade cancer is present , the passage of time can increase the risk of one of the cancer cells breaking away to enter the blood or lymphatic circulation, travelling elsewhere to start growing.
Some primary sites can be so small they may not be visible on even the best of scans.
If, however, you have secondary cancer and the primary site cannot be clearly identified by scans or other tests, you may be told you have a Cancer of Unknown Primary (CUP).
nb information on Secondary Neuroendocrine Cancer, is also available in 9 other languages, through our global advocacy partners, INCA (International Neuroendocrine Cancer Alliance), here.
How does Secondary Cancer occur?
As mentioned before, the spread of Neuroendocrine Cancer is not always a sign of rapid or aggressive cancer. To understand how cancer spreads we need to understand how cancer cells develop and what is in the body that allows it to travel elsewhere.
Secondary cancer occurs as a result of cancer cell behaviour : normal cells have a set of rules that regulate growth and behaviour, in cancer the control signals go wrong and the rules are forgotten.
In secondary cancer – that is metastases – cancer cells break away from where they first formed, travel through the blood or lymph system, and form new tumours in other parts of the body.
Cancer can spread to almost anywhere in the body. In Neuroendocrine Cancer the most common secondary sites are lymph nodes, the liver, the lungs and bones.
Cancer cells spread through the body in a series of steps. These steps include:
- Growing into, or invading, nearby normal tissue
- Moving through the walls of nearby lymph nodes or blood vessels
- Traveling through the lymphatic system and bloodstream to other parts of the body
- Stopping in small blood vessels at a distant location, invading the blood vessel walls, and moving into the surrounding tissue
- Growing in this tissue until a tiny tumour forms
- Causing new blood vessels to grow, which creates a blood supply that allows the metastatic tumour to continue growing.
Most of the time, spreading cancer cells die at some point in this process. But, as long as conditions are favourable for the cancer cells at every step, some of them are able to form new tumours in other parts of the body. Metastatic cancer cells can also remain inactive at a distant site for many years before they begin to grow again, if at all.
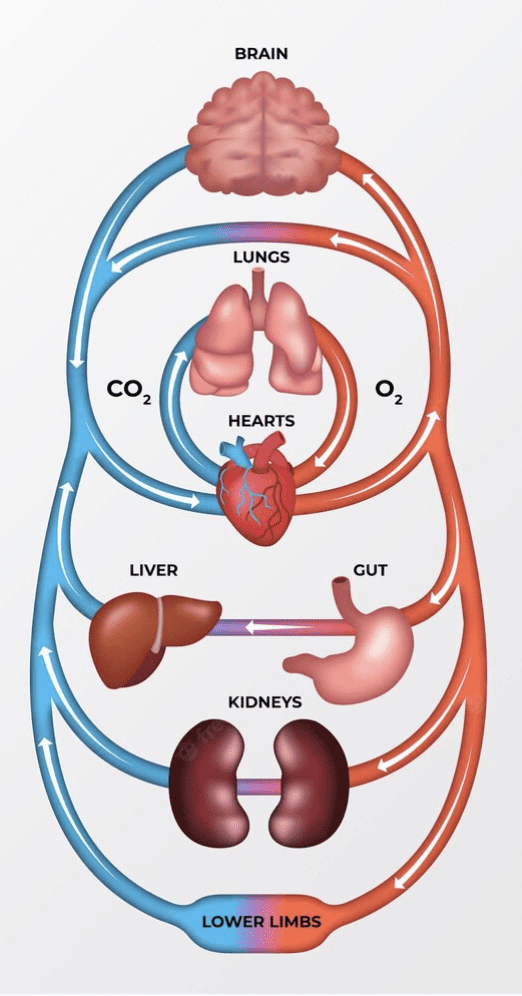
Blood Stream (Circulatory System)
All cells in the body need a system to provide them not only with oxygen and nutrients to survive, but also one that allows them to offload carbon dioxide and waste. This system is the bloodstream.
Blood is made up of blood cells and plasma. Plasma leaks out of the blood vessels and bathes your tissues and supplies the cells of your body with nutrients. Most of this plasma then drains back into the blood vessels.
Blood from the middle and lower part of the body, (including the small and large bowel) flows through the liver on its way back to the heart and lungs, and all blood flows through the lungs.
If a cancer cell enters the blood stream it is highly likely to travel to and settle into either the liver and/or the lungs – making these two of the most common sites for secondary disease.
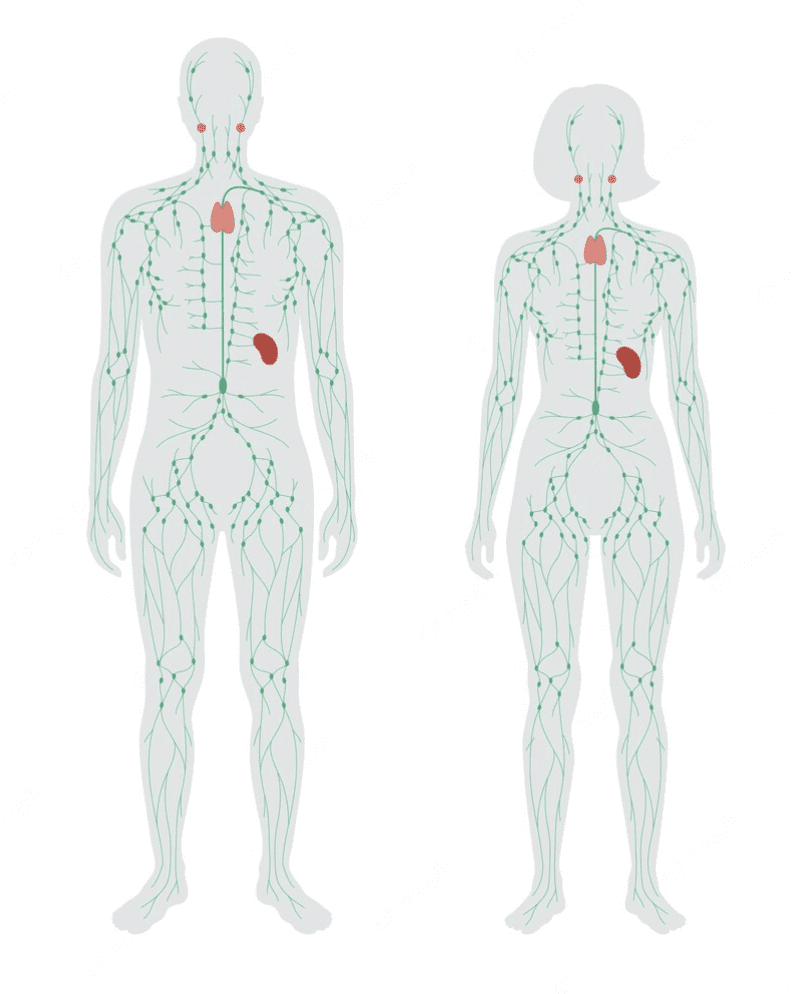
Lymphatic System
The lymphatic system is part of your immune system, which helps protect you from infection.
Lymph is formed by plasma, and contains waste products from cells – including germs, toxins and damaged/abnormal cells, along with some fats and fat soluble vitamins.
Lymphatic vessels contain lymph (like blood vessels carry blood) with lymph nodes acting as filters. These nodes contain cells that fight infection so anything that doesn’t belong in your body, including any damaged and abnormal cells are removed in the lymph nodes.
Other parts of the lymphatic system include:
- Bone marrow: is the spongy material at the centre of many of your bones. It makes all the new blood cells you need, including those that are needed to fight infection.
- Thymus: is a tiny glad that sits behind your breastbone. In children, to the age of puberty, it is responsible for producing T-lymphocytes – one of our infection fighting blood cells. As we get older it shrinks and other parts of the lymphatic system take over its job
- Spleen: sits on the left-hand side of your body, behind your stomach. It filters blood, much like lymph nodes filter lymph – and has a key role to play in how our bodies fight infection
- Tonsils and adenoids: sit at the back of your nose and throat and help protect your body against infections that enter through the mouth and nose
- Mucosa associated lymph tissue (MALT): mucosa is the soft, moist tissue that lines many parts of the body, such as the mouth, wall of the bowel, lungs, etc. MALT is part of the mucosa and helps protect the body from infections and toxins entering through a part of the body lined by mucosa.
Secondary cancer may be present at the time that Neuroendocrine Cancer is discovered – indeed this is not uncommon more than half of those diagnosed with Neuroendocrine Cancer have metastases at the time of diagnosis. For many, the primary disease may have been present for a number of months or even years, with no specific signs or symptoms occurring until the disease has spread elsewhere. For example; in Neuroendocrine Cancer of the Small Bowel it is often not until a mesenteric mass (lymph node/tissue mass near the small bowel) or liver metastases occur that more obvious symptoms are felt.
Signs and symptoms of secondary Neuroendocrine Cancer may be due to cancer site or position, for example; pain, or due to hormone excess, for example – Carcinoid Syndrome.
Small bowel neuroendocrine cancers may produce excess serotonin, however, as blood flows through the liver from the small bowel, the liver works hard to normalise hormone levels so that the excess serotonin doesn’t enter the main circulation.
However, once a small bowel neuroendocrine cancer has spread to the liver, the excess hormone produced by the metastases may bypass normal liver clearance, meaning that any excess serotonin can now enter the main circulation – clearing to symptoms such as diarrhoea, flushing, wheezing – as seen in Carcinoid Syndrome.
Secondary cancer may be present at the time that Neuroendocrine Cancer is discovered – indeed this is quite common and true for more than half of those diagnosed.
For many, the primary disease may have been present for a number of months or even years, with no signs or symptoms, until the disease has spread elsewhere. It may not be until symptoms, caused by the secondary tumour, occur that a suspicion that something is wrong is raised.
For example; in Neuroendocrine Cancer of the Small Bowel it is often not until a mesenteric mass (lymph node/tissue mass near the small bowel) or liver metastases occur, that symptoms develop – leading to diagnosis.
There are a number of tests that can be carried out to confirm a diagnosis of Primary and / or Secondary Neuroendocrine Cancer.
The type of tests you may have will be based on the type of Neuroendocrine Cancer you are thought or are known to have – and whether there is/was any evidence of secondary disease at the time of first diagnosis.
As with more common cancers, the earlier in the development of a primary cancer it is diagnosed, the higher the possibility of cure is. However, for Secondary Neuroendocrine Cancer there is no cure – but, this does not necessarily make this a terminal diagnosis.
No cure (incurable) is NOT the same as ‘terminal’, and many people living with Neuroendocrine Cancer are doing just that – living, and many are living long and well, with the support of their families, support network and specialist Neuroendocrine Cancer team.
Treatment will depend on the type (grading, functionality, etc.), position and size of your Primary Neuroendocrine Cancer. And the extent of your Secondary Cancer – where and how widely it has spread and overall how much cancer is present is important to know.
It may depend on whether you had Secondary Cancer at the time of diagnosis – or whether it has developed since – and whether you have already had treatment. If so, what effect did the treatment have – on both you and the cancer.
It will also depend on whether you have any other health concerns and / or illnesses and your general health and fitness.
One or more of the approaches below may be suggested:
- Removal of all or part of the cancer
- Control of disease, by slowing or stopping the growth of cancer
- Monitoring or Surveillance
- Palliation, or easing of, symptoms.
Surgery: To remove, partially remove or bypass neuroendocrine cancer and / or secondary sites of disease (metastases).
Non-surgical treatments include:
Somatostatin analogues (SSAs): Can be used to help regulate the secretion of hormones if abnormal levels are being produced. SSAs may also be used to slow down growth rate in low to moderate grade ‘well-differentiated’ neuroendocrine cancer (NET).
Interventional radiology: Through techniques such as embolisation or ablation – can be used to treat Neuroendocrine Cancer that may have spread to the liver and / or lung(s).
Chemotherapy: Can be given orally (in tablets) or Intravenously (through a vein) to slow tumour growth or try to reduce tumour size. This may be the first line therapy in high grade disease – particularly “poorly-differentiated’ NEC or in combination with other treatments.
Targeted Molecular Therapies: Can be given orally (in tablets) or Intravenously (through a vein) to slow tumour growth or try to reduce tumour size.
Peptide receptor radionuclide therapy (PRRT): May also be called Radioligand Therapy – uses targeted radiation to treat neuroendocrine cancer cells. Can be used in eligible patients who have had a ‘positive’ Octeotide or Gallium scan (‘receptor positive’ disease).
Radiotherapy: Can be used alongside other treatments such as chemotherapy, after surgery or on its own. It can be particularly useful for treating a single site painful bone metastasis.
Endoscopic procedure: Treatment given via endoscopy – for example, insertion of a stent to keep an airway, bile duct or part of the bowel open, if it has become blocked or narrowed by a cancer that cannot be removed.
Immunotherapy : currently of unproven benefit in most Neuroendocrine Cancers, except for Skin – that is, Merkel Cell Carcinoma (where Avelumab has received approval for use within the NHS).
Clinical studies and trials are ongoing.
Clinical Trials: Clinical research and safe new treatment development is essential to provide best care for those with Neuroendocrine Cancer – we need to know that treatments not only work but work safely. There are several phases of trial therapy – further information can be found here
Bone-strengthening treatment: Such as Bisphosphonates or other agents may be used in the management of bone metastases.
Further information on the above treatments can be found in our Treatments Section here.
Bio-psycho-social Support (BPS): Includes interventions to support you to manage physical symptoms, alongside mental health/emotional well-being and social support – and should run alongside all care, from diagnosis. It can include anything from simple medication and / or a combination of some of the treatments mentioned above to information giving and/or counselling to dietary advice to practical support including financial advice e.g. benefits and work.
Palliative Care : also known as symptom control as it refers to what may be used to alleviate or reduce the impact your cancer, other health issues and /or treatments may be having on you and your physical and mental health. It can include anything from simple medication and / or a combination of some of the treatments mentioned above to counselling and practical support. Palliative care also includes ‘end-of-life’ care.
This is not an exhaustive list – and other treatments may be offered that are tailored specifically to you. Your symptoms, your cancer, your overall health and, importantly, your choice.
All treatments decisions should be focused on the benefit you may gain from them and the impact they may have on your quality of life.
There are expert agreed guidelines regarding how and when follow up should occur, however, in practice this varies and often with good reason – follow up should be expert informed and evidence /research based but also tailored to you and what is appropriate for your best care.
Primary Site specific information is available here for further details.
Neuroendocrine Cancer Liver Metastasis & Surgery for NETs, presented by Presented by Tom Armstrong, Hepatobiliary & Pancreatic Surgeon, University Hospital Southampton.