NEUROENDOCRINE CANCER OF THE SKIN
MERKEL CELL CARCINOMA (MCC)
Merkel Cell Carcinoma – may also be referred to as MCC or Neuroendocrine Cancer of the Skin. There are 5% of all skin cancers that are considered to be rare – MCC accounts for about a third of these.
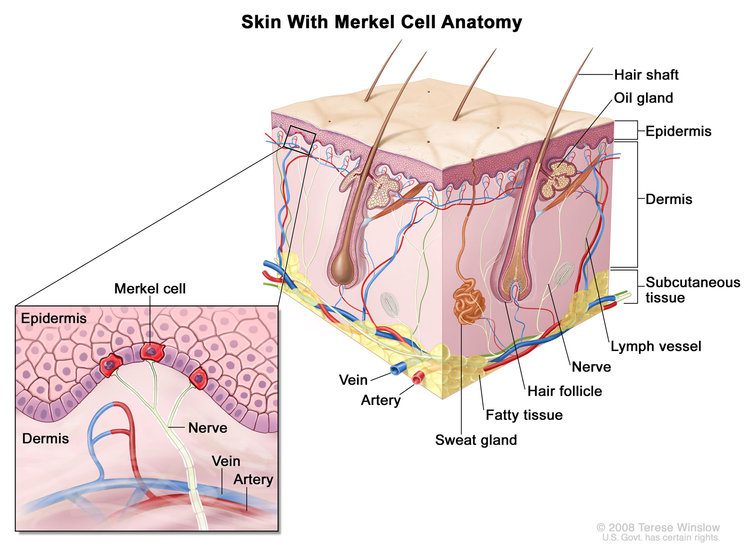
MCC is a firm, painless, skin-coloured to red-violet lump that usually develops on a sun exposed part of the skin, however it may also originate on areas of the skin usually covered by clothing – for example the genitals.
The anatomical distribution of MCCs:
- Head & neck >35%,
- Extremities (upper limbs – shoulders, arms) >20%,
- Extremeties (lower limbs – hip, legs) >25%
- Other sites (including torso, genitals and ora-nasal cavities) ~10%
- Unknown primary ~10%
Not all Merkel cell carcinomas have the same appearance, any NEW, CHANGING or UNUSUAL nodules or lumps on the skin, should be checked by a doctor / dermatologist.
It can grow rapidly (over weeks) – and may be highly aggressive, spreading to surrounding tissues and local lymph nodes – left undiagnosed or untreated – it can spread to other sites of the body including internal organs (lungs, liver and bone).
Risk factors for MCC:
Immunosuppression
– post transplant patients, those with HIV or immunodeficient conditions, or immunocompromised individuals e.g. those with blood cancers and/or those receiving immunosuppressant treatment(s).
Older than 50
– the risk of MCC development increases with age – and though the majority of those affected are over the age of 50, MCC can occur in all ages.
UV Exposure
– more than 80% of MCCs develop in sun exposed skin eg head, face, arms, hands, legs, however MCC may also develop on the torso, back and genitalia.
Fair Skin
– more than 90% develop in those with light skin tone – it is 16 times more likely to occur in those with pale skin than those with dark/very dark skin.
Merkel cell Polyomavirus (MCPyV or MCV)
– usually lives, harmlessly, on the skin in most healthy people ( >80% of the population). Once acquired, (usually during childhood) MCPyV becomes a life-long component of the skin flora. The virus can get trapped into a Merkel cell – leading to virally-induced cellular transformation – though this is rare. NB// MCC is not contagious – the virus is inactivated when it is trapped into the Merkel Cell.
Genetic Mutations
– for example mutations in tumour suppressor ATOH1 and PIK3CA genes have been found in MCC subsets.
Therefore it is important to note : previous and current medical history including medications / treatments, family history and lifestyle including work and leisure activities.
Only with early diagnosis and MCC appropriate intervention is cure possible.
In the UK in the 10 years between 1999-2008: 1515 people were diagnosed with MCC – resulting in an incidence rise from 0.1 to 0.2 :100,000
The incidence continues to increase – latest UK figures = 0.3 : 100,000 (4 people a week) – with a predicted rise to >1000 per year (3 people a day) by 2025.
There is global variation: UK/Europe 0.3 : 100,000 – approximately 4 people a week per year.
Australia 1.6 : 100,000 – approximately 8 people a week per year.
The diagnosis and management of Merkel cell carcinoma is challenging.
Patients as well as physicians may initially mistake these tumours for benign (non-cancerous) lumps, the single most common misdiagnosis being a cyst or folliculitis (inflamed hair follicles) or other skin-based lesions.
NB// MCC is rare – so other reasons for a skin lump are more likely and more commonly suspected.
In some cases, the Merkel cell tumour may arise in locations that makes it difficult to find them, delaying diagnosis, about 5% of Merkel cell carcinomas occur in the mouth, nasal cavity and throat, or the primary may be and remain unknown, making them difficult to detect in the early stages.
There are currently no specific blood tests – known as biomarkers – that can reliably predict or monitor MCC and biopsy remains the gold standard for diagnosis.
Research is underway to try to identify a reliable and effective biomarker to help improve diagnosis and surveillance.
CT (chest/abdomen/pelvis) is agreed standard practice to prove or exclude secondary disease and can help confirm staging and inform treatment planning
MRI and / or FDG-PET imaging may also be undertaken to assist in treatment decision-making.
Sentinel node biopsy +/- lymph node mapping – may be undertaken if surgery is planned.
Will depend on the site, size and stage (whether and to what extent it may have spread).
Other considerations will include overall health and the likely outcomes and potential effects of treatment.
Treatments may include one or a combination of the following :
- Surgery
- Immunotherapy
- Chemotherapy
- Radiotherapy
- Clinical trial
- Supportive care
should also be individualised according to recurrence risk, potential future options, overall health and patient preference.
- Minimise exposure to UV : Seek the shade, especially when the sun’s rays are strongest, which is usually between 10 a.m. and 2 p.m. and/or when your shadow is shorter than you, avoid sun-bathing and tanning (including use of sunbeds) and minimise risk of sunburn – especially to surgical site – and during treatment.
- Cover up with clothing, including a broad-brimmed hat and ultraviolet-blocking sunglasses.
- Use a high SPF broad spectrum (UVA/UVB) sunscreen every day on all exposed skin (even on cloudy, rainy, or snowy days) and reapply it every couple of hours while outside.
- Work with your specialist team – agree and attend appointments – for the first 2 or 3 years after treatment, this will be every 3 or 4 months. Alert them to any changes – appointments can be rescheduled if you need to be seen earlier.
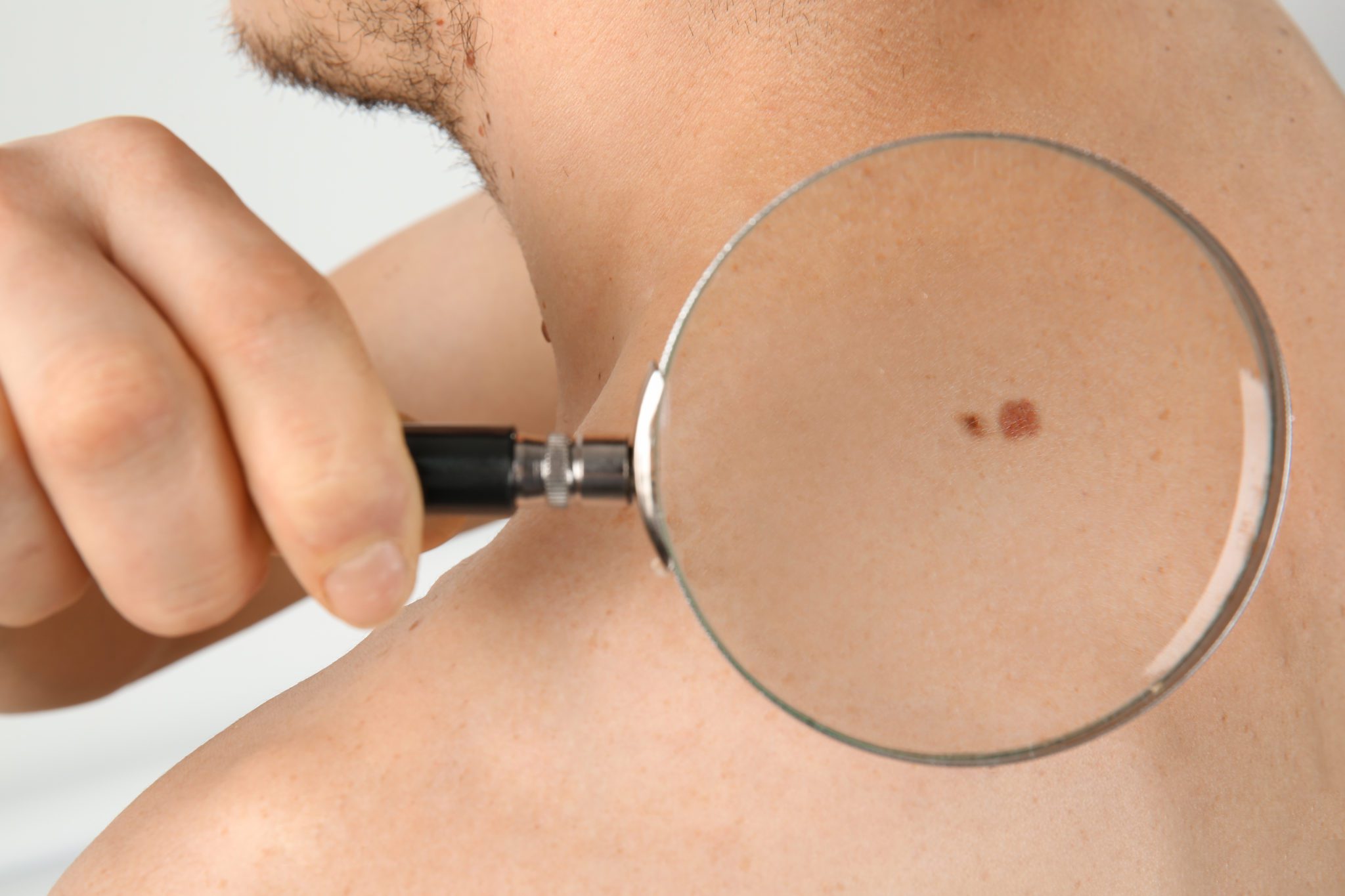
Examine your skin all over every month – being vigilant for any spot that is different from others, or that changes, itches or bleeds or is similar to previous MCC (or at same site) or other skin lesion – use ABCDEF as a helpful checklist:
A – is for asymmetry – does one part of the blemish look different from the other?
B – is for border – is the spot clearly defined ? – or is it irregular in shape?
C – is for colour – is it the same colour all over ? what colour is it?
D – is for diameter – how big is it?
E – is for evolving – is it changing in shape, size, colour ? – and how quickly?
F – is for firmness – is it a firm spot/lump? – does it hurt to touch?
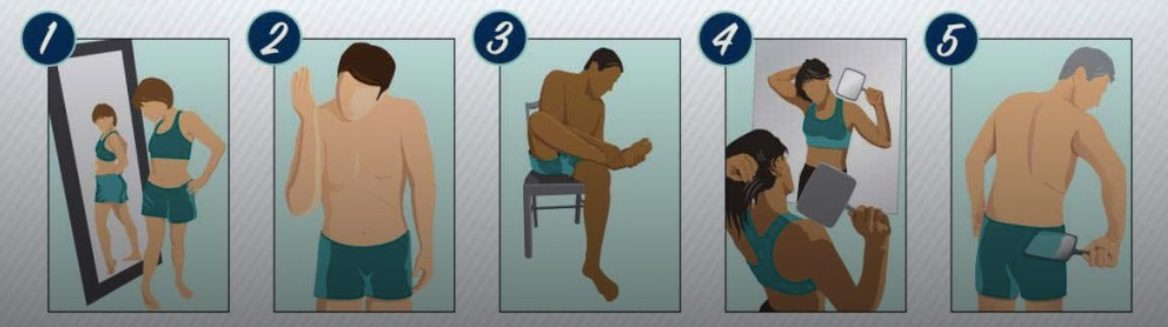
Self-exam : if you have difficulty in doing a self-exam – ask for help (e.g. partner, carer, practice nurse). Use one or both mirrors to get a clear view.
| Examine your body in a full-length mirror | Examine your body front and back in the mirror, then look at the right and left sides with your arms raised. |
| Upper limbs : arms and hands | Bend elbows and look carefully at forearms, underarms, hands and palms |
| Lower limbs : legs and feet | Look at the front and backs of your legs and feet, the spaces between your toes, and the soles of your feet. |
| Face, Head & Neck | Examine your face, including into the hairline and round to the ears. Examine the back of your neck and scalp with a hand mirror. Part hair for a closer look. |
| Back, buttocks and genitals | It may help to use a hand mirror to examine your back, buttocks and genitals |