NEUROENDOCRINE CANCER TREATMENT:
SURGERY
Aims of Surgery
In planning treatment, surgery is usually the first option considered as it may offer the only potential chance for cure (in very early stage disease) but also has a role in disease that may have spread (metastases).
There are several aims and types of surgery – all of which will depend on the type and site(s) of Neuroendocrine Cancer you have, how well you are, the risks and benefits of surgery to you and your informed consent.

Select play to watch Ryan Baron talk to us about the options, influences and progress in the surgical management of Neuroendocrine Cancer.
Remove all visible disease
If you have a single tumour, with no evidence of secondary disease (no lymph nodes or metastases) and it can be completely removed, then surgery may be a potentially curative treatment. The decision on the type and regularity of follow up will be based upon the results of the histopathology review (checking what’s been removed under a microscope).
Expert opinion is essential to assess risk of recurrence.
Remove as much as possible
Partial / Cyto-reductive / De-bulking Surgery – All of these terms refer to surgery designed to reduce the amount of cancer in your body, by removing as much as is safe to do so. This kind of surgery might involve removing:
- All or part of a primary tumour
- All or part of any secondary tumours
- All of the primary tumour and some of the secondary tumours
- Whatever can safely be removed.
This type of surgery is usually undertaken to help improve your symptoms and/or to manage the disease. It is often used in combination with other types of treatment, including; somatostatin analogues, chemotherapy, interventional radiology and/or nuclear medicine therapy.
De-bulking a tumour can improve symptoms that have been caused by the size and position of a tumour or by the release of excess hormones into the blood. It can also improve the effectiveness of other treatments, as they will be targeting a smaller amount of tumour.
Remove possible cause(s) of symptoms
Pre-Emptive/ Bypass Surgery .
Occasionally, Neuroendocrine Cancer develops too close to blood vessels and / or surrounding organs and can interfere with how these structures work – potentially leading to pain and/or other symptoms.
Removing or bypassing these kinds of tumours can help to prevent blockages and other damage, reducing the chance of extra problems developing in the future. This is known as pre-emptive or bypass surgery.
Types of Surgery Explained
Surgery is a treatment in which a part of the body is cut open so that a surgeon can repair, remove, or replace a diseased or damaged part. With any type of surgery, the length of your stay in hospital and the time it takes to recover, will depend on the type and extent of surgery you have, what your general health is like and on whether any complications occur. Your surgical team will give you full information about any surgery recommended for you.
Many hospitals produce their own information leaflets about the types of surgery they do – if you do not receive any written information, you can ask either your surgeon or specialist nurse.
Surgery is usually done one of four ways:
Keyhole Surgery
Keyhole surgery is done through very small incisions in your skin with the use of a fine tube with a light on the end (known as a fibre optic light source). The surgeon carries out the operation by using special instruments inserted through the tube. Keyhole surgery may cause less pain and reduce your length of stay in hospital (when compared to open surgery), and though it is used for an increasing number of conditions – having keyhole surgery will depend on the site and type of cancer you have. If keyhole surgery is offered as the best option for you, you may also be alerted to the possibility that open surgery may happen instead – especially if the surgeon cannot remove, debulk or bypass your cancer through the keyhole procedure.
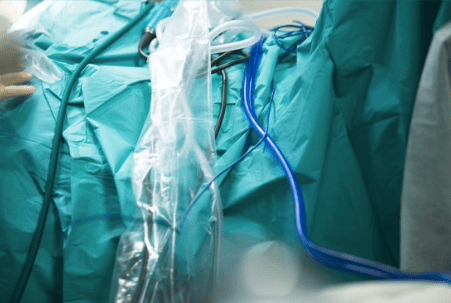
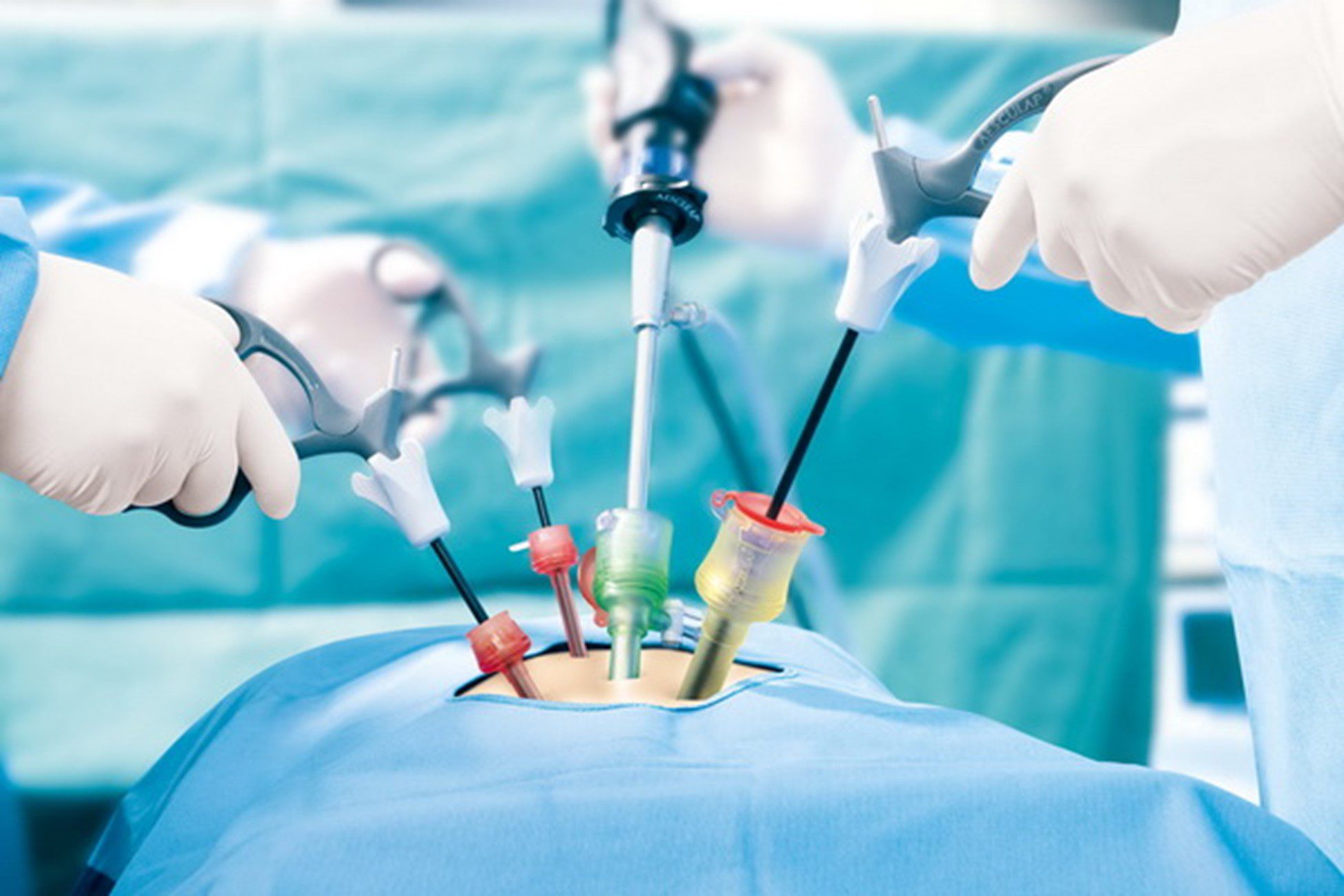
Laparoscopic
Laparoscopic surgery is similar to keyhole surgery but refers especially to operations performed inside the abdomen and in the peritoneum (the lining of the abdomen).
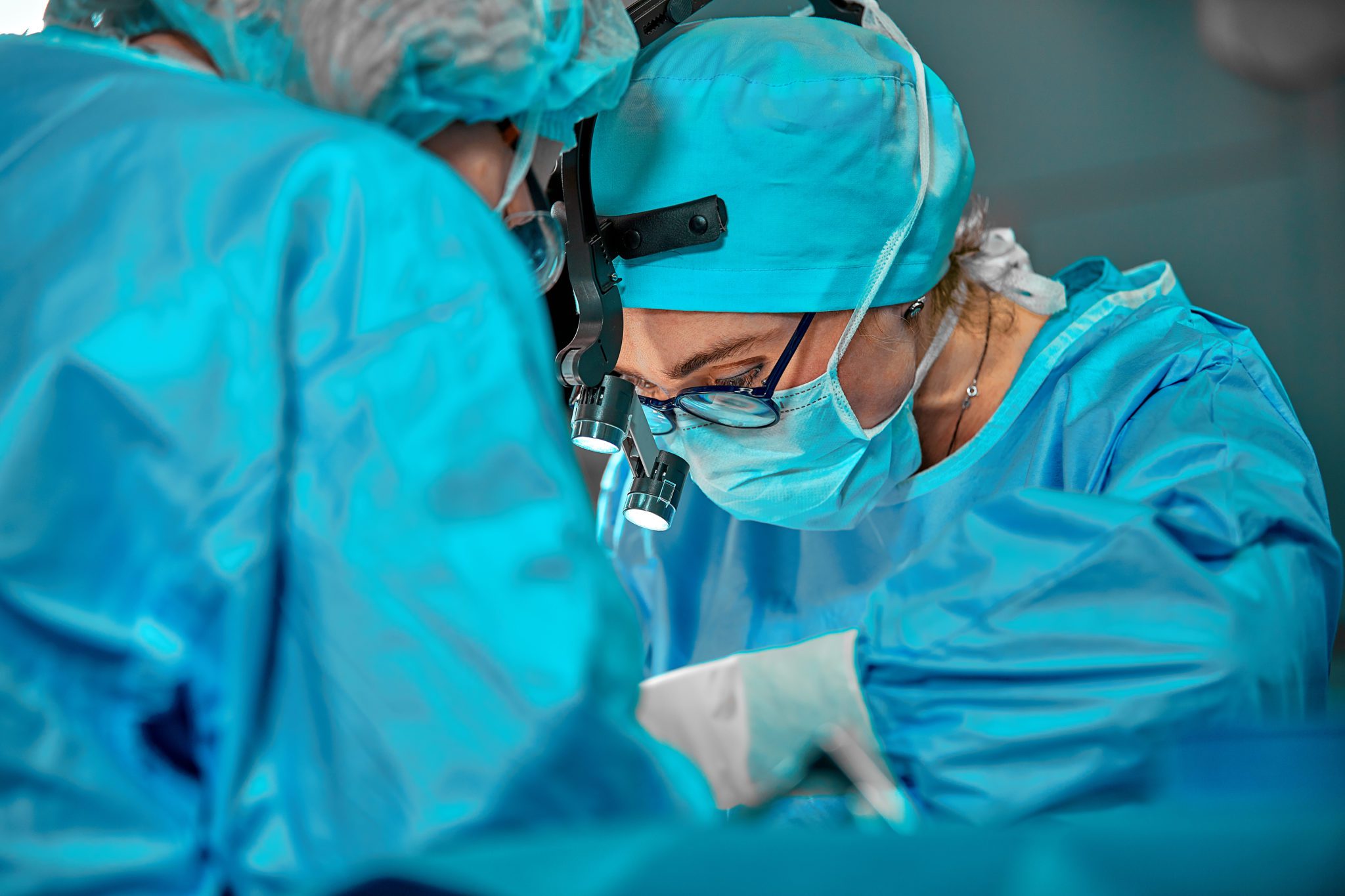
Open Surgery
Open surgery is the most common type of surgery and characterised by a cut (incision) into the body to allow the surgeon to remove, de-bulk or bypass your cancer – staples or stitches will be used to close the incision.
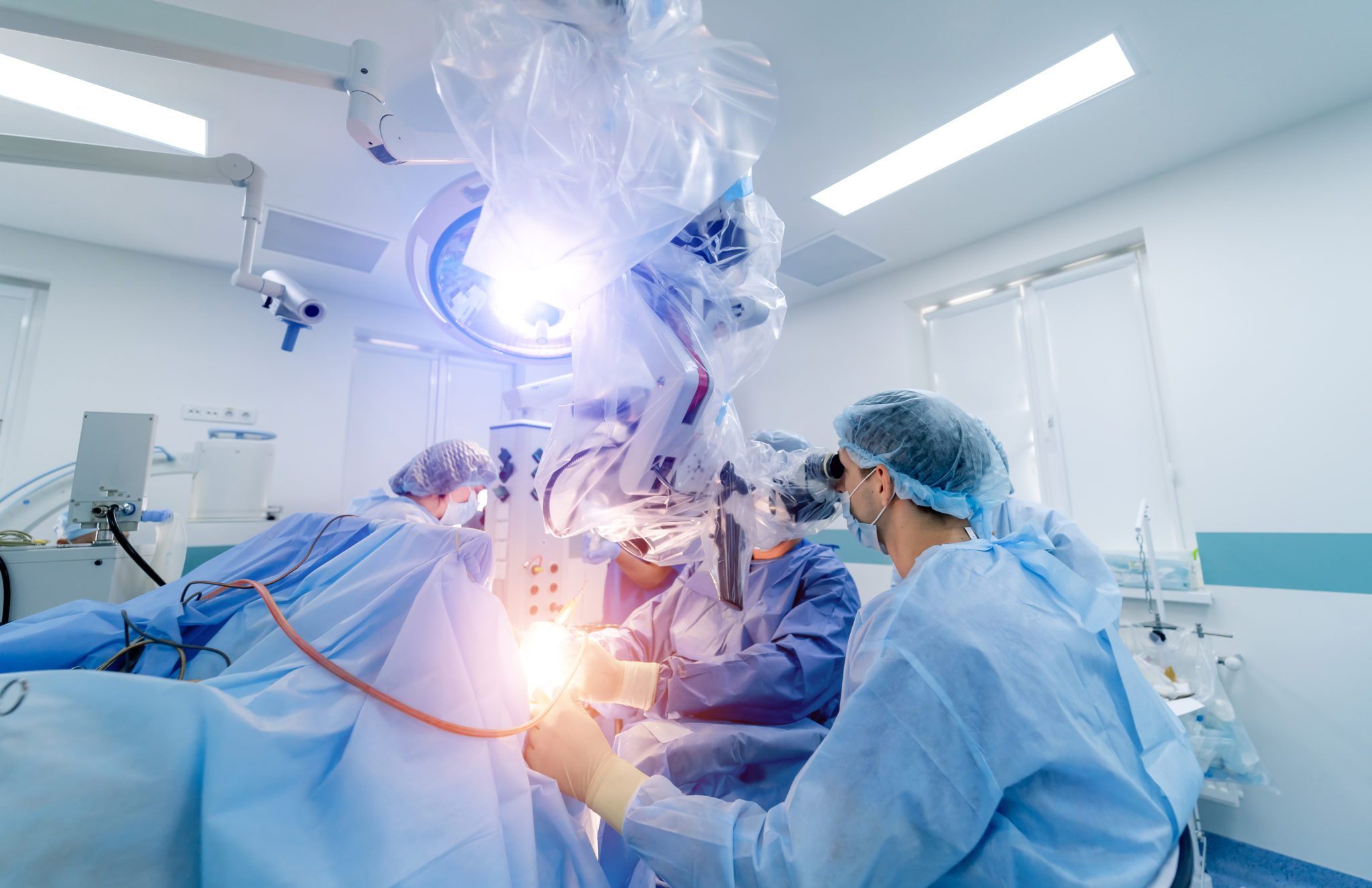
Robotic
Robotic surgery uses small incisions, as in keyhole or laparoscopic surgery, to allow the surgeon to to use several specifically designed robotic arms to carry out the procedure. This procedure is reserved for very specific types of surgery.
There are two further considerations:
Combined or Staged Surgery
You might need more than one type of surgery to treat your cancer. If this is the case for you, your surgeon will discuss whether the surgeries can be undertaken at the same time or in stages (which means you’ll have one surgery and then be given time to recover before the next one takes place).
For example; if you have a small bowel primary and liver secondary that are both suitable for removal, the surgeon will assess how much surgery would be required, how long it would take (so how long would you need to have an anaesthetic for), and the potential risks/benefits for you.

Open and Close Surgery
This term refers to surgery being started but not completed, either because of a severe deterioration in your condition during surgery or because your cancer cannot safely be removed, debulked or bypassed.
If surgery is stopped because your condition deteriorates, you’ll be given full care and time to recover .Your team will then need to review and decide, depending on the cause of your deterioration, whether it is safe to re-schedule surgery. This will be fully discussed with you.
However, if an operation is stopped because your cancer cannot safely be removed, debulked or bypassed you’ll be given full care and time to recover and then your care team will discuss alternative treatments with you.
Select play to watch Zahir Soonawalla talk to us about Surgery for small intestinal neuroendocrine tumours.
Effects of Treatment
Neuroendocrine Cancer Treatments work in a variety of ways – and whilst we wish it wasn’t the case, side-effects can occur – not will occur – but can occur. Many of these, if they happen, can be mild and manageable – others may cause an alteration or adjustment in treatment, such as reduced dose or interval – occasionally a treatment may have to stop – either temporarily (a ‘treatment break’) or permanently, because the side-effect is more severe. You may also be given treatments in a different order to what was first planned or how you may see them given in others – remember – your treatment plan will be personalised to you.
But it is only possible to deal with changes and side-effects, if you are able to talk them through with your specialist nurse or team.
If you notice a change, or don’t feel well, during or after a treatment – it may be tempting to ignore it or not mention it or wait a few weeks to see if things improve. You may be worried that if you do highlight any changes, your treatment may be stopped. However, the sooner your team knows what is happening, the sooner they can help you to deal with any changes – which will not always mean stopping treatment.
Changes or new symptoms may not always be caused by your treatment – Neuroendocrine Cancer itself can cause alterations in health – and other unrelated health issues can also occur. So, it can be helpful to know what to expect from treatment, what to look out for – and, importantly, when and who to contact if changes occur.
Potential side effects
Surgery is a treatment in which a part of the body is cut open so that a surgeon can repair, remove, or replace a diseased or damaged part. Therefore, there are risks/benefits and potential side effects and/or consequences of undergoing surgery.
These vary from person to person and may be related to several factors:
- What type of surgery you’ve had, for example, keyhole or open
- What part of the body was operated on – what was removed, debulked or bypassed?
- Length and complexity of surgery – was the aim of surgery achieved?
- Other treatments you may have received before surgery, such as chemotherapy – which may affect healing and recovery
- Your general health – level of fitness and / or other medical conditions you may be dealing with – both physically and mentally.
Your nutritional status – before , during and after surgery – may also play a role. Further information about nutrition and surgery to the digestive system can be found here.
As part of informed consent you will have received information about the risks and benefits of surgery – and may also have been given information about possible effects and / or consequences.
For example – the potential impact on fertility following surgery to either male or female reproductive organs.
There are some effects that can be common across all types of surgery:
Pain – pain is not uncommon – but hopefully, as part of your pre-assessment or surgery work-up, you will have had the opportunity to discuss likely and preferred pain relief with your surgeon and / or anaesthetist.
Numbness – you may experience some numbness along the incision site (wound). This is not uncommon in surgery where the nerves in the skin are cut during the procedure. This does not necessarily cause you any problems and often continues for quite a while afterwards. It can be a little disconcerting though, at a later date, when feeling starts to return to the area – especially if you have become used to it being numb.
Fatigue – It is not uncommon to feel fatigue after surgery – especially if you have undergone a ‘big’ or long operation. In fact research shows that you can lose more glycogen (a form of carbohydrates stored in your muscles for energy), during surgery than while training 2-3 hours for a race.
Factors that may influence the level of fatigue you may experience include:
- Level of fatigue beforehand
- Anaesthetic medications
- Pain relief
- Nutrition and appetite and the energy your body uses to help repair and recover during and after surgery Fatigue usually improves as your body recovers – but it can take time – and that time will vary from person to person.
Reduced appetite – this may be related to anaesthesia and the medications you may need to take in and around surgery – for example, some antibiotics can leave a metallic taste in the mouth, which makes everything taste odd. If you have had surgery that may affect how soon you can restart eating – talking to a dietician before and during your hospital stay – may help – especially if your surgery may require you to alter your usual diet in anyway or you have lost weight. Further information on diet and nutrition can be found here.
Bleeding/bruising – It is not unusual to experience some, slight, bleeding from the operation site – heavy bleeding requires urgent attention. Bruising may also be normal, depending on the type of surgery and whether you are receiving or self injecting blood thinning medication (anti-coagulation such as heparin)— but if it is worsening (deepening or extending) – this needs urgent medical review.
Swelling/ fluid collections / lymphoedema – the body sees surgery as an injury. The natural response to injury is inflammation – caused by a rush of protective and repair factors to the site of harm – so some swelling is to be expected. internally this is often accompanied by fluid collection in the affected area – which is why you may have a wound drain in place for a number of days after an operation to allow this fluid to drain away, rather than collect and become a possible source of infection. However, not all fluid that may gather at or near a surgical site will be directly related to this protect and recover process. In operations where lymph nodes are removed – the fluid that normally passes through them, into and out of the surrounding tissues, may not be able to drain back into the lymphatic system. This causes something known as lymphoedema – and may be a more common consequence in certain types of surgery than others – for example, following a mastectomy (breast removal) and lymph node clearance, lymphedema may occur in the arm on the same side of the body. It may also occur in certain abdominal procedures – where it may be referred to as chylous ascites (the accumulation of lymph rich fluid in the abdomen, causing swelling). If lymphedema is a possible consequence of the surgery you are to undergo, it may help to speak to a lymphoedema therapist / specialist beforehand – for additional information and advice.
Infection – is a risk of surgery but may occur elsewhere in the body, during your stay in hospital. Wound care will be provided – alongside measures to reduce the risk of either a chest or urine infection.
Altered function – Occasionally surgery may result in either temporary or permanent altered function, because the part of the body responsible for a certain function has been removed or significantly altered. For example, removing part of the pancreas may result in a temporary alteration of blood sugar control, whereas removing all of it will result in insulin-dependent diabetes (as there will be no remaining pancreas left to carry out blood sugar control).
Body Image – Surgery is a treatment the can alter the way your body looks, feels and / or functions physically, it can also have an effect on how you feel about yourself and your body – you may experience positive and / or negative changes to your self-image.
Even if you have been able to talk to your specialist team about the changes surgery may bring about – it may still take some time to re-adjust, both physically and mentally, with these changes. If you are struggling with how you feel or find yourself becoming negative or distressed by these changes – let your specialist nurse / team or GP know.
Further information about support and counselling – can be found here.
Sexual and reproductive health – how we feel about our bodies can also affect our most intimate relationships. Surgery, as mentioned above, can add a different dimension to that by resulting in either positive or negative effects on our self image. As well as our self and body image – surgery may also impact on our sexual and reproductive health by altering physical functioning – and this should be discussed with you before surgery, whether it is a definite or possible effect of surgery.
